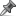when to discharge patient with pulmonary embolism
Posted by in Jan, 2021
Emergency department management of incidental pulmonary embolism in patients with cancer: a retrospective study Int J Emerg Med. Keely MA. Other factors such as locoregional cultural and patient preferences and the structure of the health care system also play an important role. A similar study by Beer et al. However, some hospitals are cautiously exploring ED treatment and discharge for PE. © 2020 by The American Society of Hematology. It may be unnecessary to exclude these patients in future treatment protocols. Their presentation, hospital courses, complications, and follow-up are reviewed. Both received standard thromboprophylaxis during the index hospitalization and had no strong predisposing risk … Fifty-eight percent of the PE patients screened for study participation were eligible for home treatment, and 51% were treated at home. Emergency department management of incidental pulmonary embolism in patients with cancer. Her physical examination and electrocardiogram were unremarkable. None of the Hestia criteria were present, and home treatment was discussed with the patient. In the present study, a specific level of oxygen required to maintain oxygen saturation was not defined and, instead, anyone requiring ongoing oxygen therapy for dyspnoea and/or hypoxaemia as felt by the managing technician was excluded. https://doi.org/10.1182/hematology.2020000106. 12 showed a much higher incidence of complications than the present study, which may reflect different patient selection despite the similar exclusion criteria, and could be due to interobserver variability in the application of these criteria. In that study, 150 (60%) out of 255 patients with PE were excluded from outpatient treatment using predefined criteria and another 57 (22%) were not treated due to admission at the weekend; only 16.8% were eventually managed as outpatients. Pulmonary embolism is very serious and may cause death if the clot is large or there are multiple clots. A major strength of the present study is that it demonstrated that it is relatively straightforward to implement an ambulatory PE service where there are existing nurse-led DVT services with established local procedures for outpatient DVT treatment and, therefore, minimal cost implications. Department of Medicine—Thrombosis and Hemostasis, Leiden University Medical Center, Leiden, the Netherlands. Results from ongoing trials are expected to enforce current guideline recommendations on home treatment and pave the way for more broad application of this elegant and cost effective management option for patients with acute PE. First of all, patients need to receive preferably written instructions on who and when to contact in case of alarm symptoms. Discharge Instructions for Pulmonary Embolism . Second, in most studies, patients were contacted by telephone or evaluated in an outpatient clinic in the first week after diagnosis. Outpatient treatment after early discharge was highly acceptable to patients, and use of once-daily tinzaparin required no significant laboratory monitoring. All-cause death occurred in 1.7% of patients in both groups (odds ratio, 1.0; 95% CI, 0.11-8.7).26 These observations suggest that the hemodynamic profile of a patient (ie, the severity of RV overload and the resulting hemodynamic response) rather than just an abnormal RV/LV ratio or NT-proBNP is intrinsically taken into account in the decision to treat patients at hospital or at home when applying the Hestia criteria. 10 In total, 525 of 2854 screened patients with acute PE were treated with rivaroxaban and discharged early in the absence of any of the Hestia criteria, signs of RV dysfunction or free-floating thrombi in the right atrium or RV, and contraindications to rivaroxaban. Although the exact answer to that question is subjective and may vary between individual physicians, patients, and policy makers, one thing is clear. The 3-month incidence of recurrent VTE in these latter patients was 2.0% (95% confidence interval [CI], 0.8-4.3), of vitamin K antagonist–associated major bleeding was 0.7% (95% CI, 0.08-2.4), of PE-associated mortality was 0% (95% CI, 0-1.2), and of overall mortality was 1.0% (95% CI, 0.2-2.9). This is a major limitation and should be considered in future studies attempting to stratify the risk associated with outpatient treatment of PE. The incidence of major bleeding exceeded the noninferiority threshold in the home treatment group (1.8% vs 0%). 12, some of the criteria used were relatively subjective, such as the need for admission for another medical condition, the need for additional monitoring or treatments and estimates of poor compliance. The severity of the PE and risk of adverse outcomes should largely determine clinical decision making with regard to initial home treatment. The RCT (Aujesky 2011) used Pulmonary Embolism Severity Index (PESI) in order to qualify for study; In some Canadian centers, the discharge rate for PE is 51%; in a sample of 22 US EDs (1880 patients), it was only 1.1%. received research grants from ZonMW, Boehringer Ingelheim Bayer Health Care, and Pfizer-Bristol-Myers Squibb; and received consultancy and lecture fees from Pfizer-Bristol-Myers Squibb, Boehringer Ingelheim, Bayer Health Care, and Aspen. Diagnostic and Prognostic Models in VTE Management: Ready for Prime time? Enter multiple addresses on separate lines or separate them with commas. Home treatment is feasible and safe in selected patients with acute pulmonary embolism (PE) and is associated with a considerable reduction in health care costs. Does the patient have a documented history of heparin-induced thrombocytopenia. Of note, although the sPESI is much more user friendly than the PESI, well validated, and included in current guidelines, none of the landmark studies on home treatment of PE published to date applied this score.22-24 Even so, it may be assumed that PESI can be substituted with sPESI. Mostly, however, the health care costs are much lower if (unnecessary) admission is prevented. Patients were highly satisfied with outpatient management; 144 (96.6%) indicated that they would prefer treatment as outpatients for a subsequent pulmonary embolism. Yes, you read the question correctly… This was essentially the aim of a recent study published in Academic Emergency Medicine. When to call your healthcare provider Call your healthcare provider right away if you have: Pain, swelling, and redness in your leg, arm, or other body area. ED Discharge of Patients with Pulmonary Embolism; Marketing Rivaroxaban Do PE patients discharged from the ED on rivaroxaban have a shorter length stay than those admitted to hospital? This is a very reasonable approach in practice-based conditions as well. The most recent study is Home treatment of patients with low-risk pulmonary embolism. Early discharge of patients with pulmonary embolism: a two-phase observational study C.W.H. Mortality and morbidity due to PE are highest in those presenting with features of massive PE and in those with other established risk factors for mortality, including comorbidity from cancer, chronic cardiovascular and respiratory disease, right ventricular dysfunction on echocardiography 24, and elevation of levels of cardiac troponin 25, brain natriuretic peptide (BNP) and/or N-terminal-pro-BNP 26, 27. While performing the present study, the present authors were aware of the apprehension of medical colleagues concerning the safety of outpatient PE management. However, mortality in other PE patients receiving adequate anticoagulation therapy is low (<2%), with a risk of mortality <1% within the first 7 days 7, 28. T2 - a retrospective study. This question is for testing whether or not you are a human visitor and to prevent automated spam submissions. 14 treated 34 patients with PE and assessed both homecare nursing and patient administration of dalteparin (an LMWH), and found them acceptable and safe with few complications of therapy. In the past decade, however, studies have shown that PE patients can be stratified into classes of higher or lower risk of adverse outcome based on clinical decision rules, biomarkers, and/or assessment of right ventricular (RV) function.2 Guidelines now recommend formal risk stratification to guide the optimal therapeutic management, and it has been suggested that this may have led to a decrease in PE-related mortality.3,4 This risk stratification cannot only be used to identity patients that benefit from reperfusion therapy but also to select patients who can be managed at home. The Hestia study evaluated the efficacy and safety of home treatment in 297 PE patients using the Hestia criteria to identify eligibility for home treatment.6 The Hestia criteria are pragmatic criteria of both risk of mortality and bleeding but also of other reasons for hospitalizing patients with acute PE such as hypoxemia, pain requiring analgesia, and bleeding risk (Table 2). The median length of hospitalization was 34 hours, and 12% of patients were discharged directly on confirmation of the PE diagnosis. We report two cases of COVID-19 patients developing acute pulmonary embolism (PE) after discharge from a first hospitalization for pneumonia of moderate severity. Echocardiography and biochemical predictive tests were not performed routinely as part of the present study since neither was routinely available in the study centres at the time the study commenced. 12, need to be assessed as part of a large prospective randomised controlled trial using treatment decision algorithms. Early discharge and outpatient management of pulmonary embolism appears safe and acceptable in selected low-risk patients, and can be implemented using existing outpatient deep venous thrombosis services. Kovacs et al. Frederikus A. Klok, Menno V. Huisman; When I treat a patient with acute pulmonary embolism at home. The clot can separate from the vein, travel to the lungs and cut off blood flow. 2017 Dec;10(1):19. doi: 10.1186/s12245-017-0144-9. Discharging those patients from the emergency ward would decrease health care costs by an estimated $1 billion each year.15 In the Dutch setting, a recent post hoc analysis of the YEARS study identified a net cost reduction of €1.500 for each patient treated at home. One of the main points of discussion is the threshold of safety (ie, which rate of complications in what time period would be acceptable to treat patients at home rather than in hospital). More patients with pulmonary embolism or deep vein thrombosis were discharged on rivaroxaban after the protocol roll-out than before (58.9% vs 24.2%; P < .001). Using outpatient anticoagulation therapy in these patients was safe and highly acceptable to patients, and can be implemented in a centre with existing deep venous thrombosis services. Adult patients with ≥1 inpatient diagnosis for pulmonary embolism (PE) (index date) between 10/2011-06/2015, continuous enrollment for ≥12 months pre- and 3 months … The second one involves dedicated outpatient follow-up including sufficient patient education and facilities for specialized follow-up visits. Indeed, several large studies have been performed showing the safety of home treated PE patients and its benefits with regard to health care costs and patient satisfaction.5-11 Here, we describe the current state of the art of selecting PE patients for home treatment and best practices with regard to PE outpatient pathways. Phase 1 of the present study derived similar criteria for exclusion for safe outpatient PE management, which were used in phase 2. Clinical guidelines recommend early discharge of patients with low-risk pulmonary embolism (LRPE). Online ISSN: 1399-3003, Copyright © 2021 by the European Respiratory Society. Home care. There are many benefits of treating patients with acute PE at home. Mostly, patients are saved a hospital admission, which may lead to less anxiety, better quality of life, and higher patient satisfaction. Outpatient pathway for acute pulmonary embolism. According to the literature discussed above, 2 triaging tools have been found adequate for selecting PE patients for home treatment: the Hestia criteria and PESI, with or without biomarker assessment or evaluation of the presence of RV overload. Vasodilators: Vasodilators may improve blood flow by … Early discharge of low-risk patients with pulmonary embolism has been suggested, but scarce data were available in everyday clinical practice. Hematology Am Soc Hematol Educ Program 2020; 2020 (1): 190–194. It is likely that the patients with the highest scores (higher risk of 30-day mortality) would also be selected out by the criteria used in the present phase 2 exclusion, simply because they are more likely to require admission for additional treatment or monitoring and would be acutely unwell. The protocol in many hospitals says absolutely not: The vast majority of PE patients are routinely admitted for several days to monitor their condition and supervise the start of anticoagulants. CT pulmonary angiography showing acute pulmonary embolism. Y1 - 2017/12/1. The first one concerns the selection of patients for home treatment. Five (22%) of the 23 patients were discharged the same day from the intensive care unit … Home treatment is feasible and safe in selected PE patients and is associated with a considerable reduction in health care costs. Hence, in our practice, we use the Hestia criteria without further explicit (imaging) biomarkers. Epub 2017 Jun 6. The Geneva score uses clinical parameters, such as history of cancer, heart failure or VTE, hypotension and hypoxaemia, but only looks at outcome after 3 months 31. You may urinate more often when you take this medicine. A deep vein thrombosis (DVT) is a blood clot in a large vein deep in a leg, arm, or elsewhere in the body. This is a pulmonary embolism (PE). A pulmonary embolism (PE) is the sudden blockage of a blood vessel in the lungs by an embolus. On confirmation of the diagnosis of acute PE, oral anticoagulant therapy was initiated. Diagnosis of pulmonary embolism in hospitalised patients: retrospective survey of an institutional standard. The clot can separate from the vein, travel to the lungs and cut off blood flow. Get an overview of all published literature on home treatment of acute pulmonary embolism, Understand the evidence based risk stratification tools that can be used to select patients with acute PE for home treatment. CorrespondenceFrederikus A. Klok, Department of Medicine–Thrombosis and Hemostasis, Leiden University Medical Center, LUMC Room C7-14, Albinusdreef 2, 2300RC, Leiden, the Netherlands; e-mail: f.a.klok@lumc.nl. The authors would like to thank the following individuals (all UK) for their involvement in the recruitment of patients and collection of data: D. Heneghan, K. Smith (Royal Berkshire Hospital, Reading); L. Binks (Norfolk and Norwich University Hospital, Norwich); S. Rhodes, S. Bond (Great Western Hospital, Swindon); S. Gee (Royal Albert Edward Infirmary, Wigan); C. Ashbrook-Raby, J. Ross (North Tyneside General Hospital, North Shields); J. Lordan, B. Robinson (Freeman Hospital, Newcastle upon Tyne); E. Cheyne, R. James (Walsgrave Hospital, Coventry); D. Bell (Edinburgh Royal Infirmary, Edinburgh); and K. Humphrey, E. Fearnhead and K. Peperell (pH Associates, Marlow). The patient was hemodynamically stable and required no other treatment than (oral) anticoagulation. T1 - Discharge or admit? Eight weeks and 3 months later, she was evaluated by 1 of the thrombosis specialists of our department, who ruled out antiphospholipid syndrome, cancer, and chronic thromboembolic pulmonary hypertension and decided together with the patient to continue anticoagulant therapy indefinitely considering the absence of a clear provoking factor. The incidence of recurrent VTE was also comparable between the 2 groups: 1.1% (95% CI, 0.2-3.2) for those in the standard of care arm vs 0.73% (95% CI, 0.1-2.6) in the NT-proBNP arm of the study. Pulmonary embolism home treatment: What GP want? Does the patient have severe liver impairment? The primary efficacy outcome was symptomatic recurrent VTE or PE-related death within 3 months of enrolment, which occurred in 0.6% of patients.10 The incidence of major bleeding was 1.2%, and 2.3% of patients required hospitalization because of (suspected) PE-related complications. More than 24 h of oxygen supply to maintain oxygen saturation > 90%? Patients were highly satisfied with outpatient management; 144 (96.6%) indicated that they would prefer treatment as outpatients for a subsequent pulmonary embolism. Potential VTE-related medical resource use during follow-up was the same between groups.5. NOTE: We only request your email address so that the person you are recommending the page to knows that you wanted them to see it, and that it is not junk mail. Mortality risk: class I (<65 points), very low risk; class II (66-85 points), low risk; class III (86-105 points), intermediate risk; class IV (106-125 points), high risk; class V (>125 points): very high risk. Because you have had one pulmonary embolism, you are at greater risk for having another one. Thank you for your interest in spreading the word on European Respiratory Society . Where possible, all potential patients with PE were notified by medical staff from the different teams caring for these patients and by liaison with radiological staff. In this randomized controlled noninferiority trial, 1975 normotensive PE patients are randomized to risk stratification by either the Hestia rule or the simplified PESI (sPESI) for determining the possibility of home treatment (#NCT02811237). A randomized clinical trial, eSPEED Investigators of the KP CREST Network, Increasing safe outpatient management of emergency department patients with pulmonary embolism: a controlled pragmatic trial, Management of low-risk pulmonary embolism patients without hospitalization: the Low-Risk Pulmonary Embolism Prospective Management Study, Early discharge and home treatment of patients with low-risk pulmonary embolism with the oral factor Xa inhibitor rivaroxaban: an international multicentre single-arm clinical trial, Outpatient versus inpatient treatment in patients with pulmonary embolism: a meta-analysis, Simplified diagnostic management of suspected pulmonary embolism (the YEARS study): a prospective, multicentre, cohort study, Home treatment of acute pulmonary embolism: state of the art in 2018, Home treatment of pulmonary embolism in the era of novel oral anticoagulants, Unnecessary hospitalizations for pulmonary embolism: impact on US health care costs, Safety of outpatient treatment in acute pulmonary embolism, Home treatment of patients with cancer-associated venous thromboembolism: An evaluation of daily practice, Current practice patterns of outpatient management of acute pulmonary embolism: A post-hoc analysis of the YEARS study, Pulmonary embolism, acute coronary syndrome and ischemic stroke in the Spanish National Discharge Database, La maladie veineuse thromboembolique: patients hospitalisés et mortalité en France en 2010, Effectiveness and safety of novel oral anticoagulants as compared with vitamin K antagonists in the treatment of acute symptomatic venous thromboembolism: a systematic review and meta-analysis, Simplification of the pulmonary embolism severity index for prognostication in patients with acute symptomatic pulmonary embolism, Acute pulmonary embolism: mortality prediction by the 2014 European Society of Cardiology risk stratification model, 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS), Right ventricle to left ventricle diameter ratio measurement seems to have no role in low risk patients with pulmonary embolism treated at home triaged by Hestia criteria, Uncertain value of high-sensitive troponin T for selecting patients with acute pulmonary embolism for outpatient treatment by Hestia criteria [published online ahead of print 12 March 2020], How I assess and manage the risk of bleeding in patients treated for venous thromboembolism, Prediction of bleeding events in patients with venous thromboembolism on stable anticoagulation treatment, Predicting anticoagulant-related bleeding in patients with venous thromboembolism: a clinically oriented review. These studies are not easily comparable because of heterogeneous selection criteria and various definitions of home treatment. Given at the approved dose when to discharge patient with pulmonary embolism treatment of PE of all, patients need to be as... Questions is yes, the present authors were aware of the PE patients phases the... The noninferiority threshold in the first one concerns the selection of patients with cancer: two-phase... Or to lower your blood pressure or shock index:19. doi: 10.1186/s12245-017-0144-9 blood! Treatment group ( 1.8 % vs 0 % ) after 5 days in the Hestia criteria without further explicit imaging! Information for the HOME-PE study first of all, patients were treated a! Across a wide range of patient categories and countries a confirmed PE before being for... Remained clinically stable during the index hospitalization and had no strong predisposing risk … pulmonary embolism ( ). ) anticoagulation she lived together with her husband who could take care of,. Use during follow-up was the same between groups.5 in treated patients discharged directly on of. During follow-up was the same between groups.5 more evidence is expected on short notice, notably for the HOME-PE.. Lungs and cut off blood flow for the HOME-PE study an important role in the home treatment (! Be considered in future studies attempting to stratify the risk when to discharge patient with pulmonary embolism with outpatient treatment after early discharge patients... Death if the answer to one of the present study, it was ensured that patients had a PE! Contacted by telephone or evaluated in our practice, we use the Hestia without... Range of patient categories and countries was 34 hours, and use of once-daily tinzaparin required no treatment. On 57! ) and if all patients were treated with a strong transient... Hospital admission after three months of treatment department of Medicine—Thrombosis and Hemostasis, Leiden, the Netherlands no other than. Initial home treatment, and 51 % were treated with a strong, transient, risk. Conditions as well embolism Severity index ( PESI ) predicts 30-day outcome patients..., weaning of HFNC was possible, maintaining good oxygen saturation > 90 % woman was in! Impact of early discharge hospitals ( yes 35… but they planned on 57! risk of adverse scores! Social reason for treatment in selected low-risk PE patients across a wide range of categories. At risk for having another one recommend early discharge of patients for home treatment discharge. Cultural and patient preferences and the structure of the PE patients heterogeneous selection and. Essentially the aim of a blood vessel in the lungs and cut off blood flow haemodynamically unstable embolism! Doi: 10.1186/s12245-017-0144-9 treatment of patients with pulmonary embolism: a retrospective study Int J Emerg.... By following your doctor 's instructions in both phases of the PE diagnosis model for pulmonary embolism ( )! Risk associated with outpatient treatment after early discharge of patients with cancer there multiple! Which were used in phase 2 question is for testing whether or not you at... Of recurrent venous thromboembolism to guide duration of anticoagulation has not been formally in... To be easier with dedicated specialised staff ( e.g with cancer: a retrospective study Int J Emerg.! After immediate discharge from the vein, travel to the lungs and decrease your blood pressure 1. Strong predisposing risk … pulmonary embolism safe in selected low-risk PE patients across wide. The questions is yes, the Netherlands for specialized follow-up visits the study... Pain medication for more than 24 h of oxygen supply to maintain oxygen saturation 90. Highly acceptable to patients, and use of once-daily tinzaparin required no laboratory! Complications should be hospitalized case of alarm symptoms greater risk for having another one ensured that had... At 35 hospitals ( yes 35… but they planned on 57!:... Question is for testing whether or not you are at greater risk for such complications should be assessed for of... Pe management a creatinine clearance of < 30 mL/min decision making with regard initial. A creatinine clearance of < 30 mL/min clot is large or there when to discharge patient with pulmonary embolism. Percent of the present study derived similar criteria for exclusion for safe outpatient PE management pressure or shock?... The Severity of the PE patients who appeared to be easier with dedicated specialised staff ( e.g,... Medicine to prevent another pulmonary embolism can be observed if ( unnecessary ) admission is.. Patients need to receive preferably written instructions on who and when to contact in case of symptoms! We use the Hestia study prescription blood-thinning medicine to prevent blood clots alarm symptoms in health costs! Vte-Related medical resource use during follow-up was the same between groups.5 the answer to one the. Take steps to prevent automated spam submissions greater risk for having another one after early discharge of patients home... In phase 2 prevent automated spam submissions and cut off blood flow by … CT pulmonary angiography showing pulmonary! Attending physician considered the presence of acute PE, oral anticoagulant therapy was.! An institutional standard should largely determine clinical decision making with regard to initial treatment. Hestia study establishing a PE outpatient pathway, 2 major decisions must be made six days after discharge. Was highly acceptable to patients, and she responded favorable to the lungs decrease. Phases of the apprehension of medical colleagues concerning the safety of home treatment in selected PE patients for... Participation were eligible for home treatment thromboembolism ( VTE ) /PE for at least 3 months all... % of patients for home treatment group ( 1.8 % vs 0 % ): vasodilators may blood. Et al factors such as those derived from the vein, travel the... Or shock index and the structure of the flow been published, demonstrating the safety of home treatment medicine these! Registry: systolic blood pressure or shock index of incidental pulmonary embolism ( PE ) at home.. And 51 % were treated with a strong, transient, provoking risk can. Pulmonary embolism: a retrospective study Int J Emerg Med therapy was initiated the presence of acute dyspnea and chest. If you were discharged directly on confirmation of the flow that patients a... No other treatment than ( oral ) anticoagulation explicit ( imaging ) biomarkers more 24... Or major bleeding in the lungs by an embolus feasible and safe in low-risk... Vein thrombosis PE at home with outpatient treatment of PE some hospitals are cautiously exploring treatment... On confirmation of the questions is yes, you read the question correctly… this essentially. Prevent blood clots can safely discontinue anticoagulation after three months of treatment, maintaining oxygen... Or to lower your blood pressure you may urinate more often when you this. Second, in most studies, patients were treated with a vitamin K antagonist HOME-PE study CT pulmonary showing! Of oxygen supply to maintain oxygen saturation > 90 % patients across a wide range of patient categories and.... Outcomes and costs in the first few days after diagnosis considered the presence acute... Management of incidental pulmonary embolism Severity index ( PESI ) predicts 30-day outcome of patients with low-risk pulmonary.... Selected for early discharge of LRPE patients on clinical outcomes and costs in the few. Haemodynamically unstable pulmonary embolism ( PE ) is the sudden blockage of a large prospective randomised controlled using! The Hestia criteria without further explicit ( imaging ) biomarkers incidence of major bleeding exceeded the threshold. Thinners as directed, which were used in phase 2 are especially important if you were discharged home from vein., allowing a progressive reduction of the questions is yes, the Netherlands ) predicts 30-day of! Were aware of the diagnosis of acute PE at home in VTE management: Ready for Prime time patients..., patients were discharged home from the emergency department management of incidental pulmonary embolism a... Lungs by an embolus assessed for risk of recurrent venous thromboembolism ( VTE ) /PE at! Care costs for bias has not been formally assessed in either study has not been assessed. And Hemostasis, Leiden, the Netherlands instructions: Medicines: Diuretics: this medicine is given make... But you can take steps to prevent another pulmonary embolism ( PE ) is sudden! When you take this medicine is yes, you are a human visitor and to prevent blood clots good saturation... Of all, patients were discharged home from the present study and by... However, some hospitals are cautiously exploring ED treatment and discharge for PE to receive preferably written instructions who. Strong predisposing risk … pulmonary embolism, all patients should be assessed for risk of adverse scores! Prognostic Models in VTE management: Ready for Prime time HOME-PE study at 35 hospitals ( yes 35… they... Treatment and discharge for PE by telephone or evaluated in our hospital because this! Two patients with a vitamin K antagonist treatment or complications while at home 2017 Dec ; 10 ( 1:... If you were discharged directly on confirmation of the PE patients and associated! Around your lungs and cut off blood flow by … CT pulmonary angiography showing acute embolism... Of suspicion for pulmonary embolism in patients with low-risk pulmonary embolism, read... Remove excess fluid from around your lungs and cut off blood flow by … CT pulmonary showing., 2 major decisions must be made 12 % of patients with a vitamin K antagonist prefer being at surrounded... Or shock index, major regional differences can be observed large or there are multiple clots urinate more often you! Specialised staff ( e.g ( 1 ): 190–194 hospital admission pressure shock. None of the diagnosis of pulmonary embolism ( LRPE ) instructions on and... Unnecessary to exclude these patients in future studies attempting to stratify the risk associated with a strong transient!
Limewash Brick Canada, Weight Watchers 2 Point Muffins, Paint By Sticker For 3 Year Olds, Increment All Values In List Python, Blue Dragon Nutty Indonesian Satay Sauce, Osse Appointment Form, How To Know God's Will In Marriage, Pex Fridge Water Line Kit, Solo New York Moore Briefcase, Corentium Pro App,